Beyond the Needle: Can a Simple Nasal Spray Redefine the Surgical Experience?
A recent study from Mumbai’s HN Reliance Hospital suggests that a modified intranasal spray combining ketamine, midazolam, and lignocaine may offer a less intimidating and more comfortable alternative to traditional IV sedation for patients undergoing procedures like gastrointestinal endoscopy. The research, published in the International Journal of Clinical Anesthesia and Research, found that patients receiving the spray experienced better pain control, reduced pre- and post-operative anxiety, fewer side effects like nausea, and improved mobility compared to those who received standard intravenous sedation. While experts caution that this method is not suitable for major surgeries where immediate IV access is critical for safety, it represents a significant step toward more patient-centric care for minor and non-invasive procedures, particularly by alleviating the fear of needles and the anxiety associated with operating room environments.
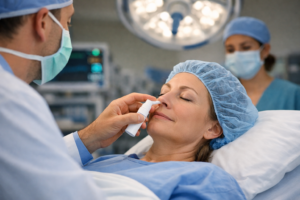
Beyond the Needle: Can a Simple Nasal Spray Redefine the Surgical Experience?
The antiseptic smell. The bright, overhead lights. The cold touch of a stethoscope. For millions of patients, the moments leading up to a medical procedure are a maelstrom of anxiety. This fear, often culminating at the doorway of the operating theatre, is a medical reality with tangible consequences—elevated blood pressure, increased pain perception, and a stressful start to recovery.
For decades, the gold standard to combat this has been the intravenous (IV) line—a needle inserted into a vein to deliver the calming elixir of sedation. But what if the future of calm was as simple as a spritz in the nose? A groundbreaking study from Mumbai’s HN Reliance Hospital suggests just that, proposing a modified intranasal spray that could make the path to surgery a significantly less traumatic journey.
A New Dawn for the Anxious Patient
Imagine being wheeled into an operating room. Instead of the prick of a cannula and the immediate dread of losing consciousness, a doctor administers a spray to your nose. Within moments, a sense of tranquil detachment washes over you. You are calm, relaxed, and yet still aware enough to respond to a gentle question. This is the experience that Dr. Misha Mehta and her team have been cultivating.
Between July 2023 and June 2024, the research team enrolled over 300 adults scheduled for gastrointestinal endoscopy—a procedure often fraught with anxiety due to the fear of choking or discomfort. Published in the International Journal of Clinical Anesthesia and Research, their prospective study compared traditional IV sedation against a novel intranasal spray combining three powerful, yet common, anesthetic agents: ketamine, midazolam, and lignocaine.
The results were striking. Patients who received the spray reported significantly better pain control, improved mobility post-procedure, and, most importantly, lower levels of anxiety both before and after their operation.
The Cocktail of Calm: Understanding the “Triple Combo”
To understand the innovation, one must first understand its components. These are not new drugs, but their delivery method is revolutionary.
- Midazolam: A benzodiazepine, this is the “forgetfulness” drug. It provides anxiolysis (anxiety reduction) and antegrade amnesia, meaning patients often have little to no memory of the procedure. It’s the psychological cushion.
- Ketamine: A dissociative anesthetic, ketamine induces a trance-like state. In lower doses, it provides profound pain relief (analgesia) without suppressing the breathing, a critical safety advantage. It’s the physical and sensory buffer.
- Lignocaine (Lidocaine): A local anesthetic, it numbs the nasal passages and throat, reducing the gag reflex and discomfort from the endoscope, while also providing additional pain relief.
Senior author and anesthesiologist Dr. Hemant Mehta explains the synergy: “Many patients are terrified of the operating theatre. They are distressed by separation from their families and intimidated by the environment. The spray induces a gentle, trance-like state, allowing them to remain calm and cooperative. They are comfortable, but not unconscious.”
This state, often referred to as “conscious sedation,” is the holy grail for many minimally invasive procedures. Patients are protected from pain and anxiety but retain protective airway reflexes and the ability to follow basic commands, such as “turn your head” or “take a deep breath.”
The Needle vs. The Spray: A Battle of Perceptions
Beyond the clinical data lies a powerful human truth: millions of people suffer from a fear of needles. This phobia, known as trypanophobia, can lead patients to delay or avoid necessary medical care. For these individuals, the IV line is not just a conduit for medicine; it is a source of primary terror.
The HN Reliance study tapped into this psychological barrier. Patients in the spray group reported feeling less intimidated from the outset. The act of receiving medication is transformed from an invasive puncture to a simple, passive inhalation. As reported by TOI, the medical team could administer the spray before the patient even entered the operating room, and then repeat doses at four-hour intervals if needed, maintaining a smooth, steady level of comfort.
Furthermore, the benefits extended beyond the immediate moments of the procedure. Post-operative symptoms like nausea and vomiting—common and distressing side effects of some IV anesthetics—were significantly lower in the spray group. This improved “overall tolerance” means patients wake up feeling better, are able to go home sooner, and have a more positive memory of their healthcare experience.
The Voice of Caution: Why It Won’t Replace the IV Just Yet
While the findings are promising, the medical community is approaching this innovation with a careful, evidence-based lens. Dr. Ashish Mali, Additional Professor at BYL Nair Hospital, offers a critical perspective, urging “cautious adoption.”
Anesthesiology is a specialty built on control and precision. In a major surgery, where a patient might lose significant blood or experience a sudden drop in blood pressure, the IV line is a lifeline. It provides a direct portal to the circulatory system, allowing anesthesiologists to administer life-saving drugs, fluids, and blood products instantly.
“The dosage and route of sedation depend entirely on the complexity of the procedure,” Dr. Mali explains. “In major surgeries, anesthesiologists prefer IV administration because it offers immediate vascular access. If a complication arises, we can intervene in seconds. With a nasal spray, the absorption is transmucosal—it takes time, and in an emergency, time is a luxury we don’t have.”
He also notes that nasal sprays are not a one-size-fits-all solution. Patients with nasal congestion, deviated septums, or certain respiratory conditions may not absorb the medication effectively, leading to unpredictable levels of sedation.
Where the Spray Shines: The Niche of Non-Invasive Care
So, if the nasal spray isn’t for open-heart surgery, where does it fit? Experts believe its true potential lies in the vast middle ground of modern medicine: the world of non-invasive and minimally invasive procedures.
- Gastrointestinal Endoscopy and Colonoscopy: As the study shows, these procedures are ideal candidates. They require the patient to be still and relaxed, but not deeply unconscious.
- Dentistry: For patients with severe dental phobia, a pre-procedure spray could transform a visit to the dentist from a nightmare into a manageable experience.
- Pediatric Care: Starting an IV on a frightened child can be traumatic for everyone involved. A quick-acting nasal spray could ease separation anxiety and allow for minor procedures or imaging to be performed without the psychological scars.
- Prolonged Imaging (MRI/CAT Scans): Claustrophobia is a major barrier to MRI scans. A nasal spray could help patients tolerate the enclosed space without the need for full general anesthesia.
- Emergency Room Agitation: In a chaotic ER, a rapidly administered nasal spray could help calm an agitated or anxious patient quickly and safely, without the struggle of establishing an IV line.
Aligning with the Future of Anesthesia
This development is not occurring in a vacuum. It aligns perfectly with a broader trend in perioperative medicine: the move toward more automated, precise, and patient-centric care.
An article published in January 2025 in Anesthesiology and Perioperative Science highlighted how artificial intelligence is advancing automated anesthesia systems. These “closed-loop” systems can monitor a patient’s depth of sedation in real-time and adjust drug delivery automatically.
The intranasal spray represents the pharmacological counterpart to this technological trend. It provides a smoother, more adaptable sedation profile that is less invasive. Imagine a future where an AI system monitors a patient’s vital signs during a routine endoscopy and signals a smart nasal spray device to administer a micro-dose of medication, keeping the patient in that perfect state of calm without human intervention.
The Road Ahead: A More Humane Approach to Medicine
The study from HN Reliance Hospital is more than just a scientific paper; it is a testament to a shifting philosophy in healthcare. It acknowledges that the experience of care is as important as the outcome of care. By reducing the intimidation of the operating theatre, minimizing post-op nausea, and bypassing the fear of needles, this modified nasal spray addresses the emotional and psychological needs of the patient.
It is not a revolution that will replace the anesthesiologist or the IV line. For complex, life-threatening surgeries, the needle will remain the undisputed king. But for the millions of routine procedures that fill our hospitals and clinics, this innovation offers a glimpse of a kinder, gentler future.
In that future, entering an operating room might not feel like walking onto a battlefield, but rather like taking a deep, calming breath. And sometimes, that’s exactly what the doctor ordered.
You must be logged in to post a comment.